Religious Restrictions vs. Quality Care: My Struggle in a Catholic Healthcare System
I’m a pro-choice nurse practitioner an d I am the only medical provider in the only clinic serving a community in the rural South. My clinic is run by a Catholic hospital. I want to share my story for a couple of reasons. One, I hope that other folks out there in similar situations (I know you’re out there!) will read this, feel a little less alone, and will keep on fighting the good fight. And two, I want to create a window into my world for those who are practicing in more liberal environments.
d I am the only medical provider in the only clinic serving a community in the rural South. My clinic is run by a Catholic hospital. I want to share my story for a couple of reasons. One, I hope that other folks out there in similar situations (I know you’re out there!) will read this, feel a little less alone, and will keep on fighting the good fight. And two, I want to create a window into my world for those who are practicing in more liberal environments.
When I moved to the South from New York City and started looking for jobs it became clear early on that I had to choose between being a comprehensive family practice provider or an abortion provider. I think that I knew that I had been practicing in a ‘bubble’ for the past few years, but I really didn’t realize what an unrealistic view I had of how primary care actually occurs in most of the country. I had an “in” for a job at an abortion clinic but I didn’t want to leave primary care. I felt a real responsibility to work in primary care, as if it would be a waste of my skills to leave it behind. I decided to take my current position because it offered some unique opportunities for me as a nurse practitioner with regard to the level of control I have over the practice as the only provider on site. The clinic was not even open yet when I was hired, so I got to pick the supplies and medications we keep in stock (with limits of course: no Depo, no IUDs, no EC, etc), I got to hire my nurse, I even was involved in picking the art we have hanging on the walls.
One of the first questions that I asked during my interview for this job was about providing basic women’s health care that included contraception. Basic, right? Contraception is legal and, especially in resource poor rural areas, control over fertility can make the difference in a family’s economic future. I was told by my administrative manager that “what happens in the exam room is none of my business, I’m sure that lots of other providers are prescribing whatever they want.” I thought this was a really weird answer at the time, but I now realize that it perfectly sums up the de facto “don’t ask, don’t tell” policy here. I reached out to my colleagues for clarification, and nobody would (or maybe could?) give me a straight answer about what was allowed or forbidden. One of my colleagues who has been prescribing birth control told me that when she provides contraception, she always gives the patient a medical diagnosis (like “Acne” or “Dysmenorrhea”) rather than use the standard v25.9 Contraceptive Management diagnosis code. So now I do that too. When a patient comes to me asking for birth control I lead them through a series of questions trying to find a reason other than fertility control to provide contraceptives, hoping that they will mention cramps or irregular periods.
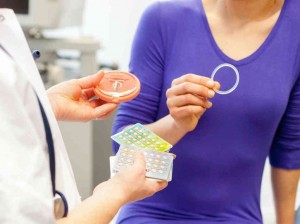 Every patient who needs birth control is a puzzle to be figured out. A time consuming, complicated puzzle. For example, if a patient wants the Depo shot, I have to call their insurance company and try to convince them to cover the Depo at the pharmacy instead of at my office because I’m not allowed to stock it. This also puts added responsibility on the patients to pick the Depo up at the pharmacy and bring it back to the clinic so I can administer it. I have been building a list of providers located within an hour of my practice who insert IUDs and contraceptive implants. These processes create a real mix of emotions in me. It is immensely satisfying to solve each of these contraceptive puzzles–I did a little dance after giving that first hard-earned Depo shot! I’m proud to spend this time to provide women the care that they need, but it does put a strain on me, my patients, and my practice.
Every patient who needs birth control is a puzzle to be figured out. A time consuming, complicated puzzle. For example, if a patient wants the Depo shot, I have to call their insurance company and try to convince them to cover the Depo at the pharmacy instead of at my office because I’m not allowed to stock it. This also puts added responsibility on the patients to pick the Depo up at the pharmacy and bring it back to the clinic so I can administer it. I have been building a list of providers located within an hour of my practice who insert IUDs and contraceptive implants. These processes create a real mix of emotions in me. It is immensely satisfying to solve each of these contraceptive puzzles–I did a little dance after giving that first hard-earned Depo shot! I’m proud to spend this time to provide women the care that they need, but it does put a strain on me, my patients, and my practice.
The relationship between religion and medical practice has created a strange environment within which I provide medical care. Talk of religion happens early and often. Every staff meeting starts with religious reflections and my clinic has been blessed by a nun. I had to sign an employment contract that said I would uphold Catholic ethics. I believe it excludes good practitioners who happen not to be Catholic by limiting the scope of their practice—you have to decide to provide birth control and risk being fired every time you do, or simply not work there. Considering how large this Catholic healthcare system is in the region where I live and work, this is definitely problematic.
I’ll admit, when I took this job I envisioned myself blowing in here and bringing in fresh ideas and making huge changes. I know now that this expectation was unrealistic. Not just because of the barriers created by my employer, but also because of the values and comfort level of many of my patients. Many of my patients have never been provided with contraception or pregnancy options, and will sometimes respond to their presentation with offense, but more often with the resignation of a decision already made by the environment in which they grew up. When I mention abortion as an option for an unplanned pregnancy, I might get a resounding “NO!” or I might get a resigned, soft “no…” that has become all too familiar. But whereas at my previous practice, I was often able to get to the bottom of that soft little “no…” I am still struggling to get there with many of my current patients. I think it’s a combination of geographical barriers (the closest abortion provider is an hour away), financial barriers (Medicaid doesn’t pay for abortions), structural barriers (at my last office I might be able to provide them with an abortion that same day!), and, finally, cultural barriers (often the patients say they don’t know anyone who has had an abortion). I’m still working on it. Another puzzle.
L.M. is a nurse practitioner working in an environment under onerous religious restrictions. L.M. must remain anonymous as any connection between their personal values and their work environment would lead to loss of employment.
